Subscription, Usage, or Custom: Which AI Scribe Pricing Model Actually Delivers ROI for Your ED?
Subscription, usage-based, or custom — the AI scribe pricing model your ED chooses directly shapes your ROI. A practical guide for emergency department administrators and CFOs on how to evaluate each model, avoid the most common cost traps, and make a financially defensible decision.

If you've reached the point of actively comparing AI scribe vendors for your emergency department, you've probably noticed something frustrating: the pricing structures don't compare apples to apples. One vendor quotes a flat per-seat monthly fee. Another charges by the minute of audio processed. A third wants a multi-year enterprise contract bundled into your EHR renewal. All three claim meaningful ROI, but their numbers are calculated so differently that putting them side by side feels almost meaningless.
This guide is written specifically for administrators and CFOs navigating that exact moment. It isn't a broad overview of AI scribing - it's a focused look at how pricing structure shapes the return you actually see, and why that distinction matters more than most buyers realize when they're making this decision.
The goal here is straightforward: by the time you finish reading, you'll have a clear framework for evaluating any AI scribe vendor's pricing model, a realistic picture of where things go wrong, and a much better sense of what to look for before signing anything.
Why Pricing Structure Matters More Than the Monthly Number
Most administrators start the evaluation process by looking at cost per seat. That’s understandable. It’s the most visible number, and it’s what finance teams are used to comparing. But in the context of AI scribing for emergency medicine, leading with sticker price is one of the most common ways departments end up with a tool that technically works but delivers almost none of the financial benefit they expected.
Here’s the reframe that changes everything: an AI scribe is not just a documentation tool. In an ED environment, where billing is governed by Medical Decision Making (MDM) complexity under the 2023 CMS E and M coding guidelines, the quality of your documentation directly determines the level of service you can bill. That means the right AI scribe is not just saving your physicians time. It’s recovering revenue that would otherwise walk out the door every single shift, invisibly, in the form of undercoded charts.
When you understand that, the relevant question stops being “what does this cost per month?” and becomes “what does this cost relative to what it recovers?”
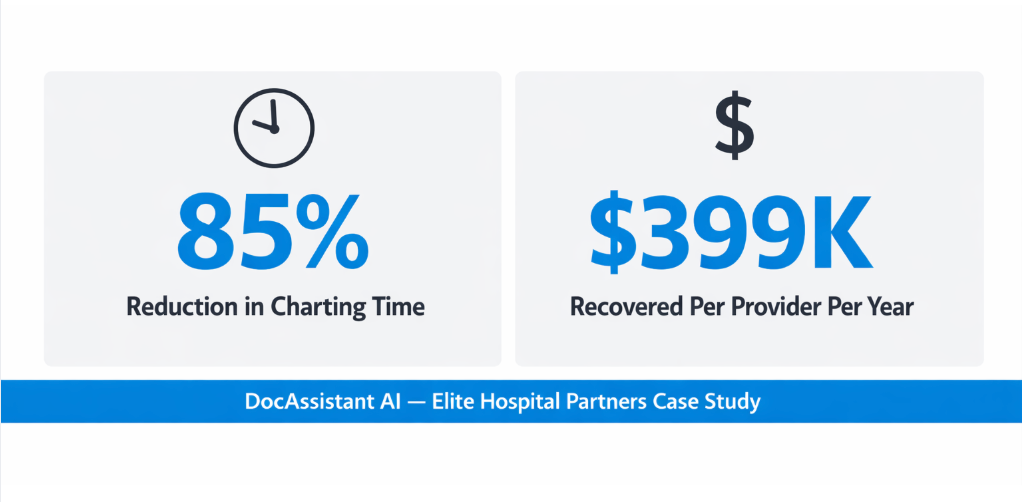
That’s the lens this guide uses. And it’s the one that led one of DocAssistant AI’s partner health systems, Elite Hospital Partners, to document an average recovery of $399,000 in lost revenue per provider per year, not as a marketing claim, but as the measurable output of aligning a pricing model with a billing recovery strategy. (For a deeper look at what that financial return actually looks like in a high-volume emergency department, see our analysis.)
The Three Pricing Models - What They Are and How They Actually Work
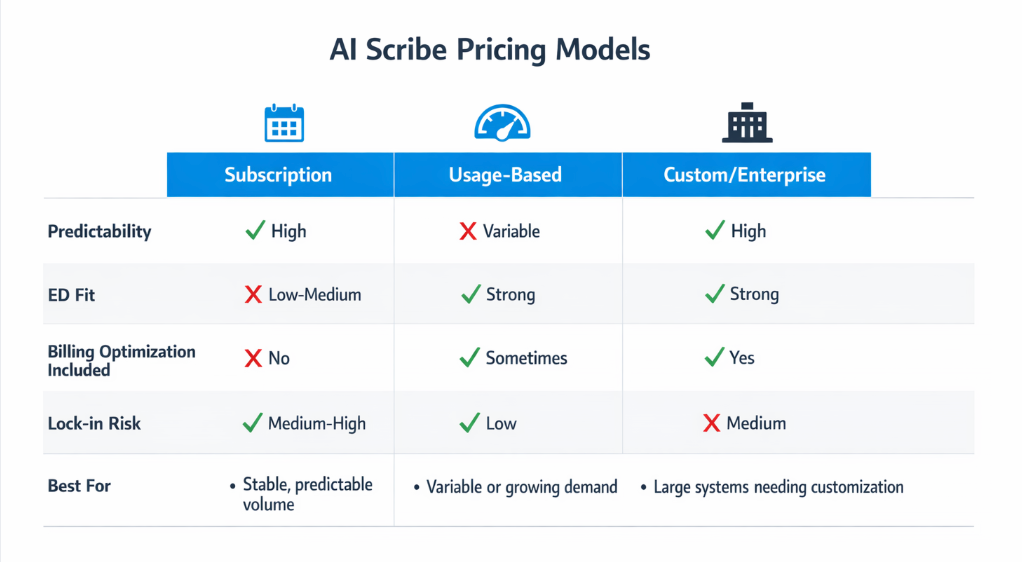
Before we get into evaluation criteria, it helps to understand the three structures you'll encounter, what each one is genuinely good for, and where each one tends to create problems in an ED environment specifically.
Model 1: Subscription / Per-Seat Pricing
This is the most common structure you’ll see. You pay a fixed monthly fee per licensed provider, typically somewhere in a range that reflects the vendor’s market positioning, and that fee stays the same regardless of how much or how little the tool gets used.
The appeal is obvious: predictable budgeting, easy to forecast, simple to explain to finance. For administrators who need clean line items, this model feels safe.
The problem in an ED context is that flat per-seat pricing creates no feedback loop between cost and value. If your 40-provider department buys 40 seats but only 28 providers actively use the tool within the first few months, a very common adoption pattern, you’re paying for 12 unused licenses while still carrying the full documentation burden those providers create. The tool becomes a budget line item, not a performance driver.
Additionally, per-seat models are often designed around broad clinical environments, not emergency medicine specifically. That means you may be paying for ambient features, specialty modules, or workflow configurations that have nothing to do with an ED, and critically, no built-in mechanism for the MDM billing analysis that determines whether you’re actually capturing the revenue each chart should generate.
Common vendors using this model include Nuance DAX, Suki, and Nabla, among others.
Model 2: Usage-Based / Per-Minute or Per-Encounter Pricing
Usage-based pricing charges you for what you actually consume, typically measured in minutes of audio transcription or number of encounters processed. In theory, this feels more aligned: you pay only when the tool is used, so cost scales with activity.
For low-volume clinical environments, this can work reasonably well. For emergency departments, it tends to create two distinct problems. First, costs become unpredictable. EDs do not have consistent volume. A mass casualty event, a flu surge, or a busy Saturday night can drive encounter counts up sharply, and your monthly AI bill reflects that variance in ways that finance teams find difficult to manage. Second, and more subtly, usage-based pricing can create a behavioral disincentive. During the busiest, most chaotic shifts, exactly when documentation support matters most, providers may hesitate to use the tool if they know every encounter adds to the bill.
Model 3: Custom / Enterprise Pricing
The third model you’ll encounter is a negotiated enterprise arrangement, often bundled into a broader health system contract, most commonly as a feature of an Epic or Cerner renewal.
On the surface, this looks attractive: it is folded into an existing relationship, the procurement team is familiar with the vendor, and the deal comes with institutional support. In practice, it carries a set of risks that are easy to underestimate at signing time.
Enterprise-bundled AI scribing tools are rarely purpose-built for emergency medicine. They are designed to check a box across multiple care settings, which means the depth of specialty-specific functionality, particularly MDM billing analysis, is typically shallow. More importantly, bundled contracts create lock-in. Two or three years into the arrangement, if the feature is deprioritized by the EHR vendor or the integration proves limited, switching costs are high enough that most departments absorb the underperformance rather than renegotiate.
According to a 2023 HFMA survey, 95% of health systems planning to purchase RCM or finance technology are actively open to “bolt-on” vendors outside their EHR system, a signal that administrators already sense bundled solutions often do not deliver the specialty depth they need.
The Evaluation Framework: 5 Questions Every CFO Should Ask
One of the most useful things an internal champion can do when bringing an AI scribe decision to leadership is arrive with a structured framework, not just a vendor recommendation, but a set of questions that any solution on the table should be able to answer clearly. Here are the five that matter most.
1. Does the pricing model align cost with actual utilization?
Flat per-seat pricing works well when adoption is close to 100% from day one. In reality, technology adoption in clinical environments rarely works that way, especially with physicians who are protective of their workflow and skeptical of new tools. Before committing to a per-seat model, ask the vendor what happens to your cost if adoption reaches 60%. If the answer is that your cost stays the same, you are taking on the utilization risk entirely.
2. Is billing optimization included, or is it a separate add-on?
This is arguably the most important question on the list. Many AI scribing tools are, at their core, transcription engines. They listen, convert speech to text, and produce a note. What they do not do, unless it is specifically built into the platform, is analyze whether the documented clinical content supports the appropriate MDM level under the 2023 CMS E and M guidelines.
That gap is where revenue disappears. Since January 2023, ED E and M coding is based on MDM complexity. History and physical exam no longer determine the billing level. (The American College of Emergency Physicians explains this shift in detail.) If your AI scribe produces a clean note but does not flag when that note supports a higher billing level than what was submitted, the revenue leakage is invisible. Ask every vendor directly whether the platform includes MDM chart-level analysis, or whether you need a separate coding tool for that.
3. What happens to your costs as volume scales?
Emergency department volume is inherently unpredictable. Any pricing model that penalizes high-utilization periods through per-encounter fees, overage charges, or usage caps is misaligned with how EDs actually operate. Confirm with vendors how costs behave at 120% of projected volume, not just at baseline.
4. Is there EHR lock-in risk?
EHR-native or EHR-bundled tools frequently tie your AI scribe capability to your EHR contract. If your EHR relationship changes, deprioritizes the feature, or raises renewal costs, your AI scribing functionality goes with it. EHR-agnostic tools, those that integrate across platforms rather than being owned by one, preserve your ability to switch without losing your documentation infrastructure.
5. How is ROI actually measured and reported back to you?
If a vendor can't show you, in clear terms, how much charting time is being saved per provider and how much revenue improvement is being driven by their billing analysis features, then the ROI claim is theoretical. Ask for outcome data from comparable ED environments before committing. If they can't produce it, that's meaningful information.
What Goes Wrong When You Choose the Wrong Model
These failure modes aren't hypothetical. They play out regularly in emergency departments that have made pricing-led decisions without working through the framework above.
The "Shelf-ware" Problem
A 40-provider department buys 40 per-seat licenses based on a compelling demo. Initial training happens, adoption numbers look okay in week one. By month three, utilization has dropped to around 60% as physicians who found the tool disruptive to their specific workflow quietly stopped using it. The department is now paying for 16 unused licenses indefinitely, while the providers who aren't using it continue to create documentation the same way they always did, slowly, after their shift, with all the coding variability that implies.
The Transcription-Only Trap
A department selects a usage-based tool with a strong per-encounter cost because it looks financially lean. The tool transcribes well. Notes get generated faster, and physician satisfaction improves. But six months in, a revenue cycle audit reveals that MDM coding accuracy hasn't changed, because the tool doesn't analyze it. The department is now more efficient at producing under-coded charts. They've automated the documentation process without capturing the billing upside. (This connects directly to the documentation errors that compound revenue loss over time - a pattern we've covered in detail here.)
The EHR Bundle Lock-In
A health system folds an AI scribe into its Epic contract renewal. The integration looks solid at signing. Two years later, the EHR vendor deprioritizes the module in favor of other development projects, updates slow down, and the ED-specific features that were promised remain partially built. The department is now locked into a contract that's difficult to exit, paying for functionality that's mediocre, with no leverage to negotiate because the AI scribe is just one line item in a much larger agreement.
Why DocAssistant AI Is Purpose-Built for This Problem
Most of the failure modes described above trace back to the same root cause: pricing models and product architectures designed for general clinical environments, not the throughput, billing complexity, and documentation demands specific to emergency medicine.
DocAssistant AI was built from the ground up for ED environments. Which means the architecture reflects how ED's actually work, not how an EHR vendor thinks they work.
Here's how it maps to the evaluation framework established above:
Does the pricing model align with utilization?
DocAssistant AI's model is structured to avoid the "shelf-ware" trap. You're not penalized for adoption variation during implementation, and the financial return scales with actual use rather than seat count.
Is billing optimization included?
Yes, and this is the core differentiator. DocAssistant AI includes a built-in MDM chart level billing analyzer that reviews documentation against the 2023 CMS E/M guidelines in real time. It identifies when a chart supports a higher billing level than was initially assigned, flagging under-coding before it becomes a revenue loss. This is not a separate add-on or a bolt-on coding tool - it's integrated into the documentation workflow.
That integration is precisely what drove the outcomes at Elite Hospital Partners. Across providers in the study, DocAssistant AI delivered an 85% reduction in charting time and recovered an average of $399,000 per provider per year in previously lost revenue. Revenue that had been there in the clinical record all along, just not captured at the appropriate coding level.
Is there EHR lock-in risk?
No. DocAssistant AI is EHR-agnostic - it integrates across platforms rather than being tied to any single EHR vendor. That means your investment in the tool doesn't become hostage to your EHR contract, and you retain the flexibility to adapt as your health system's technology relationships evolve.
Is the ROI measurable and reportable?
The $399K figure isn't an estimate - it came from a controlled implementation with a real partner health system. DocAssistant AI provides outcome reporting that finance teams can use to track charting time, coding accuracy improvement, and revenue recovery on an ongoing basis.
On compliance and audit defensibility:
DocAssistant AI holds SOC 2 Type 2 certification, which means its data handling and security practices have been independently verified. In an environment where CMS audit exposure is a real operational risk, particularly given the specificity of 2023 MDM coding requirements, that certification matters beyond marketing. It's a defensible answer to the question your compliance team will eventually ask.
Making the Case Internally: What to Bring to the Budget Conversation
If you’re the person in your organization who has worked through this analysis and is now trying to bring leadership to the same conclusion, here is the argument in its most distilled form.
The pricing model you choose is a proxy for what the vendor actually built the product to do. A tool priced around seat licenses was designed to drive broad adoption across a health system. A tool priced around encounter volume was designed to minimize friction for low-utilization environments. A tool built around billing recovery, and priced in a way that scales with the value it creates, was designed to do something fundamentally different. It captures revenue that is already embedded in your clinical care but is not making it to the claim.
The math is straightforward. At $399,000 recovered per provider per year, a 10-provider emergency department is looking at approximately $3.9 million in annual revenue recovery. Even accounting for tool cost, that is a return profile most healthcare technology investments cannot match. And unlike soft savings projections such as reduced burnout or improved satisfaction scores, recovered revenue shows up directly in financial results.
The risk of choosing wrong is not just spending money on a tool that underdelivers. It is spending money, disrupting physician workflow during implementation, and still failing to address the underlying revenue leakage. That outcome is hard to unwind, and it makes the next vendor conversation much harder.
Conclusion & Next Steps
If you’re currently comparing vendors, the most useful thing you can do before making a final decision is run the five-question evaluation framework from this guide against each solution on your shortlist. Pay particular attention to question two, whether billing optimization is genuinely integrated or an afterthought, because that is where the ROI gap between tools is widest.
DocAssistant AI offers structured demos and pilot discussions designed specifically for administrators and CFOs who are in the evaluation stage. The goal is not a sales conversation. It is to show you, concretely, how the MDM billing analyzer works in a real ED documentation workflow and what the revenue recovery modeling looks like for your provider volume and case mix.
If that's useful, request a demo here - no commitment required.
About DocAssistant
DocAssistant develops HIPAA-compliant AI documentation and medical coding solutions purpose-built for emergency medicine. Founded by practicing emergency physicians and headquartered in San Diego, California, DocAssistant combines automated clinical documentation with specialty-specific AI to reduce documentation burden, improve ICD-10 coding accuracy, and increase revenue capture for physicians, billing teams, and healthcare organizations. The company’s AI coding tool and AI scribe platform are designed to help medical billing teams, revenue cycle professionals, and clinicians work faster and document more completely. More information is available at www.docassistant.ai.
Media Contact:
DocAssistant Team
+1 619-344-0849